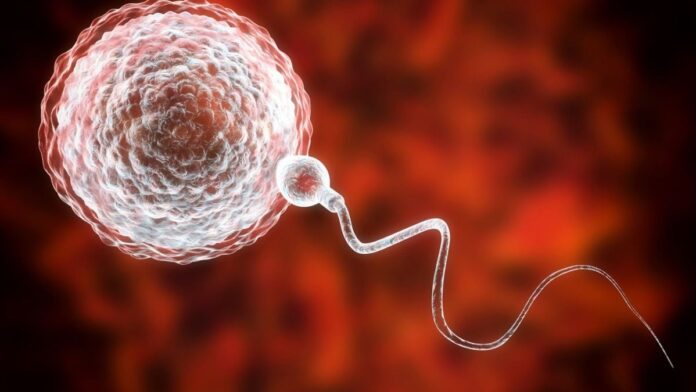
Chemotherapy and radiation are life-saving treatments for childhood cancers and blood disorders, but they come with a devastating side effect: infertility. For boys treated before puberty, traditional sperm banking is impossible because their bodies have not yet begun producing mature sperm. This leaves many young patients facing a future where biological parenthood seems out of reach.
Now, a medical team in Brussels has achieved a historic breakthrough. In the world’s first successful case of its kind, doctors restored sperm production in an adult man by re-transplanting testicular tissue that was frozen from his childhood.
The Procedure: From Freezer to Function
The patient, who remains anonymous, was born with sickle cell anemia, a genetic blood disorder. In 2008, when he was approximately 10 years old, his family consented to remove part of his testicular tissue before he underwent chemotherapy. This tissue, containing spermatogonial stem cells (SSCs) —the precursors to sperm—was cryopreserved (frozen) for future use.
Fast forward to 2022. The patient, now an adult, sought fertility treatment at the University Hospital Brussels and the Free University of Brussels (VUB). Tests confirmed that his remaining natural testicle produced no viable sperm, a condition known as azoospermia, which affects roughly one-third of men who undergo gonadotoxic treatment in childhood.
In 2025, as part of a clinical trial, surgeons performed a groundbreaking procedure. They re-introduced four grafts of his frozen childhood tissue into his adult testicle and four into his scrotum.
The results, observed one year post-surgery, are significant:
* The transplanted grafts have begun producing mature, motile sperm.
* The patient has regained the biological capacity for fatherhood, though the sperm are currently trapped within the grafts and not entering his semen naturally.
Why This Matters: A Solution for a Medical Gap
This case study addresses a critical gap in pediatric oncology. For adult cancer patients, freezing sperm before treatment is standard practice. However, prepubescent boys cannot produce sperm to freeze. Until now, there was no proven way to preserve their fertility potential.
The Brussels team pioneered the cryopreservation of immature testicular tissue in 2002. Since then, over 3,000 boys worldwide have had tissue stored, largely as a hopeful reserve for future research and potential therapies. This success validates that approach: even tissue with an “exceptionally low number” of stem cells can survive freezing, thawing, and re-implantation to function in an adult body.
“If you freeze tissue and keep cells alive, then they should have the potential. You’re putting the tissue back into the perfect environment to stimulate it. Scientifically and biologically, it makes sense. In reality, it’s still amazing.”
— Rod Mitchell, Pediatric Endocrinologist, University of Edinburgh
Next Steps and Limitations
While this is a monumental step forward, it is not yet a guaranteed path to parenthood for all patients. Several important caveats remain:
- Assisted Reproduction is Required: Because the sperm are produced in isolated grafts not connected to the sperm ducts, the patient cannot conceive naturally. He will likely need specialized laboratory procedures to retrieve sperm for in vitro fertilization (IVF).
- Longevity is Unknown: Animal studies suggest these grafts may have a short lifespan. It is unclear how long the sperm production will continue in humans.
- Safety and Health: The ultimate question is whether children conceived via this method will be healthy. Researchers plan to closely monitor embryo development, pregnancy outcomes, and the long-term health of any resulting offspring.
Veerle Vloeberghs, a fertility specialist at Brussels IVF, emphasized that while the procedure offers new options, it does not guarantee success for every patient. However, it transforms a previously hopeless situation into one with tangible possibilities.
Conclusion
This world-first transplant proves that fertility preservation for prepubescent boys is scientifically viable. While further research is needed to establish long-term safety and efficacy, the procedure offers a beacon of hope for thousands of young cancer survivors who were previously told they could never have biological children.