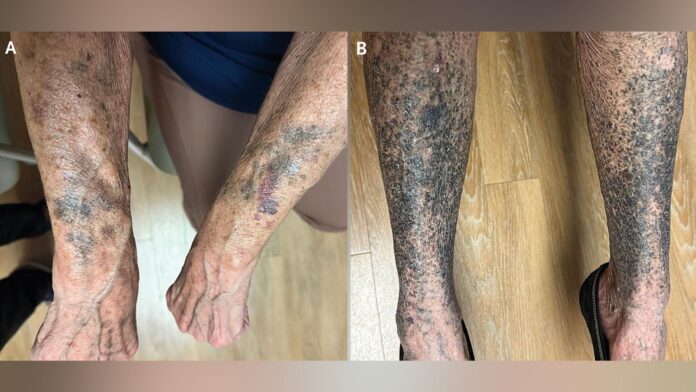
A 68-year-old woman in the United States recently presented doctors with a puzzling dermatological mystery. Over the span of six weeks, her arms and legs developed alarming dark patches. These were not ordinary bruises; the discoloration ranged from deep blue and purple to jet-black, spreading from her legs to her forearms and even appearing on the sides of her tongue.
The key to solving this diagnostic dilemma lay in the patient’s recent medical history. Two weeks prior to the onset of these symptoms, she had begun taking minocycline, an oral antibiotic commonly prescribed to treat rosacea. While minocycline is effective at reducing the inflammation and bumps associated with rosacea, it carries a rare but visually striking side effect: minocycline-induced hyperpigmentation.
Understanding the Reaction
The patient was diagnosed with Type II minocycline-induced hyperpigmentation. This specific classification is defined by blue-gray discoloration appearing on the extensor surfaces of the arms and legs—areas of “normal” skin rather than previously injured or inflamed tissue.
Minocycline can cause three distinct types of skin discoloration, each with unique characteristics:
* Type I: Blue-black discoloration appearing on scarred or inflamed skin, typically on the face.
* Type II: Blue-gray patches on healthy skin of the limbs (the patient’s diagnosis).
* Type III: Muddy-brown pigmentation on areas of the body exposed to sunlight.
Why This Case Is Significant
While hyperpigmentation is a known side effect of minocycline, this case stands out for two primary reasons: speed and visibility.
Typically, Type II and Type III hyperpigmentation are dose-dependent, meaning the drug must accumulate in the body over months before visible changes occur. However, this patient developed symptoms within just two weeks of starting a standard 100-milligram daily dose. This rapid onset challenges the conventional understanding that long-term use is required for these specific types of discoloration to manifest.
The prevalence of this side effect is also a subject of debate. One frequently cited study suggests that up to 28% of rosacea patients taking minocycline may experience hyperpigmentation, though this figure comes from a small sample size. The true incidence remains unclear, highlighting a gap in long-term safety data for this widely used medication.
The Science Behind the Stain
The exact mechanism behind minocycline-induced hyperpigmentation is complex and not fully understood, but current medical theory points to how the body processes the drug.
- Metabolite Accumulation: As minocycline breaks down, it creates metabolites that bind with iron.
- Immune Cell Capture: These iron-drug complexes are absorbed by macrophages (a type of immune cell) and accumulate in the skin.
- Melanin Interaction: The drug may also stimulate melanocytes (pigment-producing cells) to create more melanin, while simultaneously binding to existing melanin. This creates dark pigment complexes that linger in the skin tissue.
Treatment and Prognosis
The immediate treatment for this condition is straightforward: stop taking the medication and avoid sun exposure. Ultraviolet light is known to exacerbate hyperpigmentation, making the dark patches more pronounced and harder to fade.
In this patient’s case, doctors advised discontinuing minocycline. Six months later, the discoloration on her limbs had faded somewhat, but it remained visible. This aligns with broader medical reports, which indicate that once hyperpigmentation sets in, it can take months to years to dissipate. In severe cases of Type III hyperpigmentation, the discoloration may be permanent.
Conclusion
This case underscores the importance of monitoring patients on long-term antibiotic therapy for rosacea. While minocycline is a valuable tool for managing inflammation, its potential to cause significant, slow-fading skin changes requires careful consideration. For patients and doctors alike, it serves as a reminder that effective treatment must be balanced against potential aesthetic and physiological side effects, particularly when those effects can persist long after the medication is stopped.